Introduction
Glioblastoma and Current Treatment Challenges
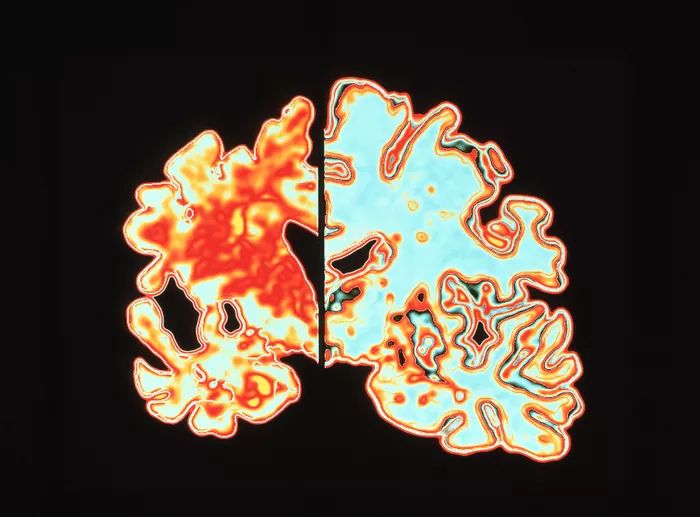
Glioblastoma (GBM) is the most aggressive malignant primary brain tumor in adults and is characterized by rapid proliferation, infiltration into surrounding brain tissue, and high rates of recurrence. Despite advances in neuro-oncology, survival outcomes remain poor. The current standard of care is surgical removal of as much tumor tissue as possible, followed by radiotherapy with concurrent Temozolomide chemotherapy, and results in a median overall survival of approximately 15 months (Latzer et al., 2024). Recurrence is nearly universal due to tumor heterogeneity, immune evasion, and resistance to therapy. Because of these limitations, researchers have increasingly explored immunotherapy as a potential treatment strategy for glioblastoma.
Personalized Neoantigen Vaccines
One promising immunotherapeutic approach is the use of personalized neoantigen vaccines. Neoantigens are peptides derived from tumor-specific somatic mutations that can be recognized as foreign by the immune system. Personalized peptide vaccines are developed by sequencing tumor DNA, identifying mutated peptides predicted to bind patient-specific Human Leukocyte Antigens (HLA) molecules, and vaccinating the patient with these peptides to stimulate CD4+ and CD8+ T-cell responses (Latzer et al., 2024). Because neoantigens are unique to tumor cells, they may allow for more targeted immune responses with reduced off-target toxicity. Prior Phase I/Ib work has established early proof of concept for this approach in GBM: Keskin et al. (2019) demonstrated that neoantigen-specific T cells induced by personalized peptide vaccines could migrate into the intracranial tumor itself, and Johanns et al. (2024) showed that multi-region tumor sequencing could expand the targetable neoantigen pool and drive clonal expansion of tumor-directed effector T cells. Latzer et al. (2024) investigates the feasibility and clinical outcomes of using personalized neoantigen peptide vaccines in a large real-world cohort of glioblastoma patients.
Purpose of the Study
The primary goal of the study by Latzer et al. (2024) was to evaluate whether personalized neoantigen-derived peptide vaccines could be feasibly produced and used in clinical practice for patients with glioblastoma. Specifically, the authors sought to assess the feasibility of vaccine production and administration, evaluate the safety of repeated peptide vaccinations, measure immunogenicity by detecting vaccine-induced T-cell responses, analyze clinical outcomes such as overall survival, and compare outcomes with propensity-matched historical control cohorts (Latzer et al., 2024).
Methods
Cohort
The study analyzed 173 patients with IDH-wildtype glioblastoma who received personalized peptide vaccines between 2015 and 2023 (Latzer et al., 2024). The cohort included both newly diagnosed patients treated before disease progression and patients treated after recurrence. Most individuals had previously received standard therapy involving radiotherapy and temozolomide (Latzer et al., 2024).
Vaccine Design
The personalized vaccine development pipeline involved several steps: sequencing tumor tissue to identify somatic mutations, predicting potential neoantigens capable of binding patient HLA molecules using computational algorithms, synthesizing peptides corresponding to predicted neoantigens, and administering repeated peptide vaccinations over several months (Latzer et al., 2024). Across the study cohort, 2,955 peptides were synthesized in total, with each vaccine containing a median of 19 peptides targeting different tumor mutations (Latzer et al., 2024). This multi-epitope strategy is consistent with emerging best practices, as targeting a broader neoantigen repertoire may help counteract immune escape– when the immune system fails to recognize and destroy a pathogen– driven by tumor heterogeneity (Johanns et al., 2024).
Immune Monitoring
Immune responses were evaluated using peripheral blood samples collected during treatment. Flow cytometry and intracellular cytokine staining were used to detect activated CD4+ and CD8+ T cells responding to vaccine peptides (Latzer et al., 2024). Patients were categorized as immunological responders or non-responders depending on the magnitude of the T-cell response observed following vaccination (Latzer et al., 2024).
Key Findings
Safety
The therapy exhibited a favorable safety profile. Most adverse events were mild (grade 1–2), with only four grade-3 reactions reported and no grade-4 toxicities observed (Latzer et al., 2024). These findings suggest that peptide vaccination is generally well tolerated.
Immune Response
Among patients with available immune monitoring data, approximately 90% developed detectable T-cell responses to at least one neoantigen peptide (Latzer et al., 2024). Many patients generated responses against multiple peptides, indicating broad immune activation. This rate of immunogenicity is notable given GBM’s typically immunosuppressive behavior (Keskin et al., 2019).
Survival Outcomes
Median overall survival for the vaccinated cohort was 31.9 months from diagnosis, which is substantially longer than typical survival estimates for glioblastoma (Latzer et al., 2024). Furthermore, patients exhibiting multiple vaccine-induced T-cell responses demonstrated a median survival of approximately 53 months, compared with 27 months for patients with weaker or absent immune responses (Latzer et al., 2024).
Interpretation of Results
The results suggest that personalized neoantigen vaccines are both feasible and capable of eliciting significant immune responses in glioblastoma patients. The strong correlation between vaccine-induced immune responses and survival outcomes indicates that immune activation may contribute to improved clinical outcomes (Latzer et al., 2024).
However, because the study was observational and not randomized, the authors emphasize that causal relationships cannot be definitively established (Latzer et al., 2024). Improved survival in this cohort could reflect patient selection, concurrent therapies, or other unmeasured confounders rather than a direct effect of vaccination.
Limitations
The study used a retrospective observational design, which limits the ability to attribute survival improvements directly to vaccination (Latzer et al., 2024). The patient population was heterogeneous, including individuals with both newly diagnosed and recurrent tumors. Additionally, many patients received other treatments during the study period, which may have influenced outcomes (Latzer et al., 2024). Finally, immune monitoring data were not available for all participants, introducing the possibility of systematic bias in the immunogenicity findings (Latzer et al., 2024).
A particularly important limitation is the socioeconomic dimension of patient access. Personalized neoantigen vaccines are incredibly expensive, with costs estimated at over $100,000 per patient (Zhang et al., 2024). Patients who can access this treatment outside of a formal clinical trial are, by definition, those with substantial financial resources or exceptional insurance coverage. Wealthier patients tend to have better baseline health, greater access to supportive care, and higher rates of treatment at high-volume academic medical centers– all factors that independently predict better outcomes in GBM. This represents a meaningful form of selection bias that is not accounted for in the analysis and that substantially tempers the interpretability of the survival data.
Future Directions
Despite these limitations, the study by Latzer et al. (2024) represents one of the largest real-world analyses of personalized neoantigen vaccines in glioblastoma. The findings suggest that individualized cancer vaccines are feasible, safe, and capable of inducing tumor-specific immune responses at real-world scale. These results support further investigation of personalized immunotherapy strategies in controlled prospective clinical trials to determine whether neoantigen vaccines can meaningfully improve survival in glioblastoma patients (Latzer et al., 2024).
The study by Latzer et al. (2024) provides encouraging evidence that personalized neoantigen peptide vaccines may represent a promising strategy for treating glioblastoma. By stimulating tumor-specific immune responses, this approach could potentially complement existing therapies and improve patient outcomes. However, randomized clinical trials will be necessary to confirm the therapeutic benefit of this strategy, and future work must also grapple seriously with the equity implications of a treatment that currently remains accessible only to a privileged subset of patients.
References
Iamukova, L., Alferova, E. (2026) Personalized Cancer Vaccines in the Clinical Trial Pipeline. Asia-Pacific Journal of Clinical Oncology 22, no. 3: 362–368. https://doi.org/10.1111/ajco.70006
Johanns, T. M., Garfinkle, E. A. R., Miller, K. E., Livingstone, A. J., Roberts, K. F., Rao Venkata, L. P., Dowling, J. L., Chicoine, M. R., Dacey, R. G., Zipfel, G. J., Kim, A. H., Mardis, E. R., & Dunn, G. P. (2024). Integrating Multisector Molecular Characterization into Personalized Peptide Vaccine Design for Patients with Newly Diagnosed Glioblastoma. Clinical cancer research : an official journal of the American Association for Cancer Research, 30(13), 2729–2742. https://doi.org/10.1158/1078-0432.CCR-23-3077
Keskin, D.B., Anandappa, A.J., Sun, J. et al. (2019). Neoantigen vaccine generates intratumoral T cell responses in phase Ib glioblastoma trial. Nature 565, 234–239. https://doi.org/10.1038/s41586-018-0792-9
Latzer, P., Zelba, H., Battke, F. et al. (2024). A real-world observation of patients with glioblastoma treated with a personalized peptide vaccine. Nat Commun 15, 6870. https://doi.org/10.1038/s41467-024-51315-8
Wu, D. W., Jia, S. P., Xing, S. J., Ma, H. L., Wang, X., Tang, Q. Y., Li, Z. W., Wu, Q., Bai, M., Zhang, X. Y., Fu, X. F., Jia, M. M., Tang, Y., Chen, L., & Li, N. (2024). Personalized neoantigen cancer vaccines: current progression, challenges and a bright future. Clinical and experimental medicine, 24(1), 229. https://doi.org/10.1007/s10238-024-01436-7